Abstract
Background: Administrative wait times reflect the time from the decision to treat until surgery; however, this does not reflect the total time a patient actually waits for treatment. Several factors may prolong the wait for colon cancer surgery. We sought to analyze the time from the date of surgical consultation to the date of surgery and any events within this time frame that may extend wait times.
Methods: We retrospectively reviewed the cases of all adult patients in Ontario aged 18–80 years with diagnosed colon cancer who did not receive neoadjuvant therapy and underwent resection electively between Jan. 1, 2002, and Dec. 31, 2009. Wait times were measured from the date of surgical consultation to the date of surgery. We chose a wait time of 28 days, reflecting local administrative targets, as a comparative benchmark. We performed univariate and multivariate analyses to identify variables contributing to a waits longer than 28 days. Variables were analyzed in continuous linear and logistic regression models.
Results: We included 10 223 patients in our study. The median wait time from initial surgical consultation to resection was 31 (range 0–182) days. Age older than 65 years had a negative impact on wait time. Preoperative services, including computed tomography, cardiac consultation, echocardiography, multigated acquisition scan, magnetic resonance imaging, colonoscopy and cardiac catheterization also significantly increased wait times. Wait times were longer in rural hospitals.
Conclusion: Preoperative services significantly increased wait times between initial surgical consultation and surgery.
Timely access to health care is a priority for patients with cancer and their physicians and has led to interest in the length of time patients wait at the various steps during their treatment. With the important role surgery plays in the treatment plan for many patients with cancer, several stakeholders have focused on the clinical significance of the wait times that these patients experience.
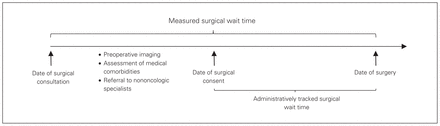
Colon cancer is a prominent cancer for which surgical wait times may impact outcomes. In North America, colon and rectal cancer has an incidence of 48.8 cases per 100 000 and is the second most common cause of cancer-related death.1,2 The diagnosis is generally confirmed by colonoscopy, often after a lengthy period experiencing vague symptoms. These symptoms or the diagnosis of cancer will prompt a referral to a surgeon, who may manage further work-up necessary to arrive at a decision to treat and to obtain consent for resection. In many jurisdictions, administratively tracked surgical wait times include only the date from the decision to treat until the date of surgery (Fig. 1). This metric may neglect the time taken for diagnosis and staging; as a result, actual wait times may be much longer than what is captured by administrative data.3–10 Furthermore, several events may occur after the date of diagnosis which, although important in surgical planning, may negatively influence the date of surgery. Such events may include preoperative imaging, endoscopy, assessment of medical comorbidities and referral to specialists before consenting for surgery, all of which may increase surgical wait times during the patient journey.11
The continuum of the patient journey.
Currently, there are no established benchmarks delineating acceptable wait times for cancer surgery. In Ontario, existing administrative targets for operative wait times (from date of decision to treat until date of surgery) prioritize patients with debilitating symptoms or aggressive cancer to a 14-day wait time goal and prioritize asymptomatic patients with an invasive cancer to a 28-day wait time goal.12,13 Most patients with colon cancer are perceived to match the criteria for the 28-day wait time goal.
As time of diagnosis is not incorporated into the administrative wait time and is difficult to determine through administrative and physician billing databases, it is not currently possible to analyze wait times from the time of clinical diagnosis, symptom development or positive screening test to the time of surgery. Therefore, our goal was to analyze the time from initial surgical consultation to the time of surgery and to analyze all events and required workup that take place in this preoperative period. To calculate this more patient-centred metric, we used administrative data, which have been shown to correlate well with abstracted data from patient charts when calculating wait times.14 Our objective was to track the flow of patients with colon cancer through the current management system and define any barriers to care that may exist within the treatment process.
Methods
We performed a population-based retrospective review of administrative databases kept by the Institute for Clinical Evaluative Sciences (Toronto, Ont.). We included adult patients (aged 18–80 yr) with resectable colon cancer who were surgically treated in Ontario between Jan. 1, 2002, and Dec. 31, 2008. Patients were identified using the Ontario Cancer Registry (OCR), in which they were registered at the time of surgical specimen or cancer biopsy. The Registered Persons Database is a roster of all beneficiaries of the Ontario Health Insurance Plan (OHIP) and was used to collect the following demographic information: patient age, sex, local health integration network (i.e., geographical region), year of diagnosis and rurality. We calculated the Charlson Comorbidity Index (CCI) score using Canadian Institute for Health Information discharge data with regards to comorbidities reported during hospital admissions 1 year before surgery. We used Statistics Canada data to calculate income quintile based on median incomes by postal code of residence. Exclusion criteria were invalid OHIP number, not receiving colon resection within 6 months of inclusion in the OCR, admission for emergency surgery, rectal or rectosigmoid cancer, metastatic disease, receiving chemotherapy or radiation before surgery and not receiving a surgical consultation.
Surgical wait times were measured from the date of surgical consultation to the date of surgery. We recorded the following data for each patient: anesthesia consultation, cardiology consultation, computed tomography (CT) scan, magnetic resonance imaging (MRI), bone scan, thallium stress test, echocardiogram, multigated acquisition (MUGA) scan, cardiac catheterization, colonoscopy/flexible sigmoidoscopy, resection setting (academic v. community hospital), right-sided cancer (International Classification of Diseases, Tenth Revision, Clinical Modification [ICD-10-CM] codes C18.0, C18.2, C18.3, C18.4, C18.5) versus left-sided cancer (ICD-10-CM codes C18.6, C18.7) and hospital volume (i.e., average yearly number of surgical consultations during the study period).
Statistical analysis
We chose the administrative wait time goal of 28 days as a comparative benchmark, but expected the time frame being studied to be longer than this administrative goal (Fig. 1). We performed univariate and multivariate analyses to identify variables contributing to a wait time longer than 32 days. Variables were analyzed in continuous linear and logistic regression models. We considered results to be significant at p < 0.05. All analyses were performed using SAS software version 9.2 (SAS Inc.).
Results
We identified 10 223 patients with colon cancer who were surgically treated during the study period and met inclusion criteria. Cohort demographic and clinical charateristics are summarized in Table 1. The number of patients treated more than doubled over the study period (Table 1). The median age of the cohort was 68 years; 46% were women. There was a significant difference in wait time between patients with right-sided and left-sided colon tumours (p < 0.001). Most patients lived in an urban setting (83%), and these patietns had shorter wait times than those living in rural areas (p < 0.001). Most patients were treated at community hospitals (76%), and these patients had longer wait times than those treated at academic institutions (p < 0.001). Wait time was significantly associated with the region where patients underwent resection (p < 0.001). Importantly, the wait time increased each year over the study period (Table 1). The median wait time overall was 31 (range 0–182, interquartile range [IQR] 16–59) days. Wait time decreased with increasing hospital volumes (Table 1). The median hospital volume was 161 (IQR 113–254) cases per year.
Demographic and clinical characteristics of the cohort, and median wait times
We also examined data for median wait times according to preoperative tests and consultations (Table 2). Not surprisingly, wait times were longer when a test or consultation was done. Preoperative tests with the largest effect on wait times were cardiac catheterization (60.5 d), colonoscopy/ sigmoidoscopy (22 d) and thallium stress test (22 d; Table 2).
Median wait times for preoperative tests and consultations
Factors for multivariate and continuous analyses were grouped according to patient, tumour, institutional and pre-operative factors. Data from multivariate analysis are summarized in Table 3. No tumour factors had a negative impact on wait time. The only patient factor having a negative impact on wait-time was age older than 65 years (p < 0.001). Surgical resection at a rural institution had a negative impact on wait time (p < 0.001). Preoperative factors and consultations associated with a negative impact on wait times included CT scan (p < 0.001), cardiac consultation (p < 0.001), echocardiogram (p < 0.001), MUGA scan (p = 0.009), MRI (p < 0.001), colonoscopy (p < 0.001) and cardiac catheterization (p < 0.001). On continuous analysis (Table 4), preoperative factors extended the wait time by several days: CT scan (3 d), lower volume hospital (5 d), echocardiogram (9.5 d), bone scan and cardiology consultation (12 d), MRI (16 d), colonoscopy (23 d) and cardiac catheterization (30 d). No wait time differences by income quintile were found. In patients younger than 50 years, wait time was reduced by 4 days.
Multivariate analysis for wait times longer than 32 days versus wait times of 32 days or shorter
Multivariate analysis for wait times (in days) as a continuous generalized linear model
Discussion
Up to 80% of patients with cancer will require surgery.15,16 Surgical resection of a tumour often represents the entry point into the cancer treatment system, and wait times for surgery can impact the entire patient journey.17 Delays in tumour resection may have adverse effects on outcomes18–20 and create additional psychosocial stress for patients.21–25 Specifically for surgical resection, the patient journey is influenced by how long it takes for symptoms to prompt testing as well as the time required to conduct appropriate testing, the time to surgical consultation, preoperative staging assessments, discussion at multidisciplinary care conferences and, finally, the wait for surgery.4,9,17 Wait times are also influenced by the volume of other patients requiring preoperative testing, surgery, the availability of limited physical and human resources and the organization of local health care delivery.16,17 These factors can create barriers to timely provision of care for patients with cancer. Conversely, some waiting in any system is inevitable. The only way to minimize wait times is by having excess capacity in the system. However, excess capacity creates an inefficient system and may create overutilization.12 The challenge facing policy-makers is to establish reasonable wait times balancing medical risk with cost-effective availability of resources to deliver not only necessary surgical care for patients with cancer, but for all patients in the system.12
We selected a cohort of patients with resectable, non-metastatic colon cancer who did not require neoadjuvant therapy to analyze surgical wait times because the management is relatively linear and tends toward a less complicated treatment plan. Patients with rectal cancer or metastatic disease were excluded, as these patients have more treatment options, including neoadjuvant chemotherapy and chemo-radiation. In this setting, we have found large variations in wait times for patients with colon cancer. As such, patients such as those with esophageal, gastric or rectal cancers, who require a more complex assessment and neoadjuvant treatments can be assumed to have even more lengthy waiting periods from diagnosis to surgery.
Of the 10 223 patients with diagnosed resectable colon cancer, more than half had a surgical wait time longer than the 28-day goal, with a median wait time of 31 days. These results can be interpreted in different ways. If this 28-day goal is exceeded by 3 days, this may not have an adverse impact on outcomes. However, the upper portion of the IQR was 59 days, extending more than 30 days beyond the 28-day goal. Simunovic and colleagues26 found that, while disease-specific effects on survival by wait time was nonsignificant, the risk of death in patients with colon cancer was greater when the time interval from decision to treat until surgery was 22 days or more versus 1–7 days (hazard ratio [HR] 1.1, 95% confidence interval [CI] 1.0–1.2, p = 0.013) and when the time from diagnostic test to surgery was 43 days or more versus 1–14 days (HR 1.2, 95% CI 1.1–1.3, p = 0.003). As cardiac testing appeared to cause major delays in the time to surgery in our cohort, the results may be confounded by cardiac or other comorbidities that we were not able to fully account for in this analysis. Regardless, an upper IQR of 59 days leaves substantial room for improvement. Tumour factors did not add to the wait time, while preoperative investigations added the most time. Computed tomography did not add a great deal of extra wait time (3 d), whereas MRI, bone scan, colonoscopy, cardiology consultation and particularly cardiac catheterization added greatly to wait times.
Academic centres had a shorter wait timed than community centres. High-volume centres, which most academic centres are, also had shorter wait times than low-volume centres. These results seem counterintuitive, as high-volume academic centres are thought to be busy centres with longer wait times. Simunovic and colleagues26 demonstrated from Surveillance, Epidemiology and End Results (SEER) Program data for 1993–96 that treatment at high-volume centres in the United States predicted longer wait times. The results from our cohort contradict this finding. Caution must be exercised when comparing data from 2 different eras and between 2 different health care systems, as various confounding factors may weaken the comparison. However, factors such as a larger surgical faculty and appropriate support staff, including anesthesiologists and registered nurses; more operating rooms; and the infrastructure to conduct all preoperative testing at 1 facility suggests that high-volume academic centres in our study jurisdiction (Ontario) may have greater capacity and efficiency than low-volume community hospitals and are therefore able to achieve shorter wait times.
We found considerable variation in median wait times by geographical region. Overall, 86% of hospital admissions for colon cancer surgery took place within the regions of the patients’ residence at the time of diagnosis, with wide variations among regions.27 Regions with the lowest median wait times were located in heavily urbanized areas. There was also significant crossover between regional boundaries for colon cancer surgery in urbanized areas, such that more than 16% of residents crossed into adjacent regions for surgery.27 Furthermore, up to 44% of patients travelled into one of these heavily populated, hospital-dense regions for colon cancer surgery.27 In contrast, the regions with the highest median surgical wait times were sparsely populated and spread across vast geographical areas. It may be more difficult for patients in these rural areas to travel large distances to a small number of hospitals (compared with highly urbanized hospital-dense regions in smaller geographical areas), and these rural areas do not have adjacent regions to share the demand for colon cancer surgery. This supports prior findings that use of health care services is greater in areas where services are available, and differences among regions that do and do not provide health care services may reflect local availability of services, patterns of disease and patient referral patterns.28
Socioeconomic status did not predict a longer surgical wait time in this cohort of patients with colon cancer. These results contradict those of studies examining socioeconomic status and access to health care in other countries.29,30 Specifically in cancer care, differences in socioeconomic status have been found for several different types of cancer31–34 and may influence cancer-related outcomes. Canada’s public health care system mandates equal access for all patients, regardless of socioeconomic status. Our results suggest patients of differing socioeconomic status have equal access to care.
A concerning finding is that median wait times steadily increased during our study period. The median wait time was 25 days in 2002 and increased to 35 days by 2008. There were 6600 new cases of colon cancer in Ontario in 200235 compared with 8000 in 2008.36 The combination of an aging population and the success of colorectal cancer screening campaigns have likely both contributed to this rise in incidence. Unfortunately, it does not appear that the increase in the number of patients requiring colon cancer surgery has been met with an increase in surgical capacity to meet the demand.
Preoperative testing can add weeks to the delay to receiving cancer care within the current system. In response to these delays, diagnostic assessment programs (DAPs) have been established for rapid diagnosis of various cancers. These DAPs are characterized by facilitated access to comprehensive diagnostic services, multidisciplinary consultative expertise, patient information resources and psychosocial support.37 However, many DAPs are institution-based. Establishing guidelines for necessary preoperative workup on a regional level or devising navigational flow charts to avoid unnecessary tests in an effort to streamline the referral and processing system could increase efficiency and reduce not only the surgical wait time, but also services overused by physicians. Diagnostic assessment programs could include dedicated imaging slots and colonoscopy slots to ensure timely access, creating a central organizing/processing system of referrals. In addition to DAPs, dedicated hospital beds and operating room capacity protected from intake of patients requiring emergency surgery combined with optimized postoperative care pathways reduced surgical wait times for joint replacement surgery;38 such a strategy may produce similar results for other procedures, such as colon cancer surgery.
Our study was conducted using the date of surgical consultation to the date of surgery as a more patient-centred wait time definition. In Ontario, the decision to treat to the date of surgery is currently tracked to monitor and evaluate the association between system capacity and the demand for surgery to help plan for appropriate system capability.12 However, this method of tracking wait times does not account for the full wait that patients experience. The decision to treat date is often distinct from the date of diagnosis or the date of surgical consultation and follows the date after all necessary preoperative investigations are completed. Thus, it should not be influenced by any of the factors that we examined. Future directions may seek to shift the definition of wait times toward a more patient-centred metric. A shift toward administrative recording of the date when referral for symptoms occurs, or the date of positive screening test, is more representative of the starting point in the patient journey. Greater awareness and efforts to improve this time interval may in turn improve the patients’ overall satisfaction with their treatment journey and improve outcomes.
Conclusion
In this retrospective analysis of 10 223 patients, we found that the wait time for essential preoperative services and consultations significantly increased the wait time experienced by patients. Older age, rural address, treatment in low-volume hospital and year of diagnosis were also independent predictors of a longer wait time for colon cancer surgery. Identifying factors affecting wait times will be critical to targeted administrative interventions, especially in the jurisdiction we examined, as wait times for colon cancer surgery appear to be increasing over time.
Acknowledgements
This work was generously supported by Colon Cancer Canada. N.G. Coburn has received funding through the Ontario Ministry of Health and Long-Term Care (MOHLTC; Career Scientist Award). C. Law is supported by the Hanna Family Research Chair in Surgical Oncology. This study was supported by the Institute for Clinical Evaluative Sciences (ICES), which is funded by an annual grant from the Ontario MOHLTC. The opinions, results and conclusions reported in this paper are those of the authors and are independent from the funding sources. No endorsement by ICES or the Ontario MOHLTC is intended or should be inferred.
Footnotes
This paper was presented in full at the Canadian Society of Surgical Oncology Annual Meeting, April 2011.
Study performed at the Institute for Clinical Evaluative Sciences, Toronto, Ont.
Competing interests: None declared.
Contributors: A. Gillis, A. Smith, C. Law and N.G. Coburn designed the study. A. Gillis and N.G. Coburn acquired the data, which all authors analyzed. M. Dixon wrote the article, which all authors reviewed and approved for publication.
Funding: Colon Cancer Canada.
- Accepted April 16, 2013.