Abstract
Background: Acute cholecystitis is one of the most common diseases requiring emergency surgery. Ultrasonography is an accurate test for cholelithiasis but has a high false-negative rate for acute cholecystitis. The Murphy sign and laboratory tests performed independently are also not particularly accurate. This study was designed to review the accuracy of ultrasonography for diagnosing acute cholecystitis in a regional hospital.
Methods: We studied all emergency cholecystectomies performed over a 1-year period. All imaging studies were reviewed by a single radiologist, and all pathology was reviewed by a single pathologist. The reviewers were blinded to each other’s results.
Results: A total of 107 patients required an emergency cholecystectomy in the study period; 83 of them underwent ultrasonography. Interradiologist agreement was 92% for ultrasonography. For cholelithiasis, ultrasonography had 100% sensitivity, 18% specificity, 81% positive predictive value (PPV) and 100% negative predictive value (NPV). For acute cholecystitis, it had 54% sensitivity, 81% specificity, 85% PPV and 47% NPV. All patients had chronic cholecystitis and 67% had acute cholecystitis on histology. When combined with positive Murphy sign and elevated neutrophil count, an ultrasound showing cholelithiasis or acute cholecystitis yielded a sensitivity of 74%, specificity of 62%, PPV of 80% and NPV of 53% for the diagnosis of acute cholecystitis.
Conclusion: Ultrasonography alone has a high rate of false-negative studies for acute cholecystitis. However, a higher rate of accurate diagnosis can be achieved using a triad of positive Murphy sign, elevated neutrophil count and an ultrasound showing cholelithiasis or cholecystitis.
Acute cholecystitis is one of the most frequent conditions requiring emergency general surgery. Many studies show early cholecystectomy results in better outcomes, a shorter length of stay in hospital and lower health costs.1–6 Therefore, it is imperative to make a diagnosis early in the patient’s presentation to the emergency department with the help of an accurate clinical assessment and appropriate diagnostic tests.
Intravenous cholangiography and oral cholecystography were the imaging tests of choice for diagnosing acute cholecystitis until they were supplanted by transabdominal ultrasonography in the early 1980s.7,8 More recently it has been recognized that ultrasonography is very accurate for diagnosing cholelithiasis but less so for diagnosing cholecystitis, with reported positive predictive values (PPV) of 37%–88% and negative predictive values (NPV) of 38%–86%.9–13 Computed tomography (CT) has similar pitfalls, with the possibility of false-positive and false-negative diagnosis of acute cholecystitis.10,12 Clinical signs, such as a positive Murphy sign, arrest of inspiration during palpation of the right upper quadrant14 and laboratory investigations are also diagnostically helpful but not definitive in the diagnosis of acute cholecystitis when interpreted in isolation.15
The Vernon Jubilee Hospital is a busy 148-bed regional hospital that serves a local population of about 66 000 and a regional population of more than 120 000. The primary objective of this study was, in the interest of quality assurance, to determine the accuracy of ultrasonography in the diagnosis of acute cholecystitis in particular and also of cholelithiasis and choledocholithiasis at our community hospital. Secondary objectives were to determine if a combination of ultrasonography and other variables would increase the diagnostic accuracy and to examine the surgical outcomes of emergency cholecystectomy at our hospital. This was a collaborative effort between the departments of surgery, diagnostic imaging and pathology.
Methods:
We examined the cases of all patients presenting to the Vernon Jubilee Hospital who required emergency cholecystectomy during a 1-year study period (Mar. 1, 2011, to Mar. 1, 2012). All surgeons consented to their charts being reviewed for this study, and patient confidentiality was strictly maintained. Charts were reviewed in accordance with the institution health records policy on quality assurance and improvement.
We recorded patient demographic characteristics, clinical parameters, length of stay in hospital, outcomes, imaging results and pathology results in a Microsoft Excel 2010 spreadsheet. All imaging results were reviewed by a single radiologist (I.M.), and all pathology results were reviewed by a single pathologist (J.D.). The radiologist and pathologist were blinded to the each other’s results.
Murphy sign was considered positive if this was documented by the emergency physician or the attending surgeon or if there was a sonographic Murphy sign (tenderness while compressing the gallbladder with the ultrasound transducer under visualization)16 in the ultrasound report.
The diagnosis of cholecystitis on an ultrasound was made if 2 major criteria or 1 major and 2 minor criteria were met.13 Major criteria included sonographic Murphy sign, gallbladder wall thickening greater than 3 mm and pericholecystic fluid. Minor criteria included intra- or extrahepatic biliary dilatation and gallbladder hydrops (transverse diameter > 5 cm).
All ultrasonography examinations were performed on either the Phillips IU22 platform with 5 MHz C5 curved array transducers or the General Electric Logic 9 with 5 MHz curved array transducers. Colour flow doppler was used to identify increased flow in cases of gallbladder wall thickening greater than 5 mm.
The diagnosis of cholecystitis on CT scan was made if there were 2 or more of the following criteria present: gallbladder distention, wall thickening greater than 4 mm, mucosal hyperenhancement or pericholecystic fat stranding or fluid.17
All CT imaging was performed on the Toshiba Aquillion 64 slice, with multiplanar reformat images based on 0.5 mm isotropic voxels. Scans were performed with intravenous iodinated contrast when indicated and when renal function parameters (serum creatinine and estimated glomerular filtration rate) were within acceptable limits.
The gallbladder tissue was fixed in 10% neutral buffered formalin (4% neutral buffered formaldehyde) for a minimum of 24 hours before prosection. Representative sections were placed into tissue cassettes and placed on a Sakura VIP6 automated tissue processor with a total processing time of 13.5 hours. The tissues were manually embedded on a Sakura Tissue Tek instrument and sectioned at 4 μm intervals on a Microtom 355 microtome. The tissue was placed on Snowcoat glass slides, stained with Leica Surgipath Gill II hematoxylin and eosin on a Sakura Prisma automated stainer and cover-slipped on a Sakura Film automated cover slipper.
Acute cholecystitis is clinically defined by acute exacerbation of abdominal pain with right upper quadrant tenderness associated with fever and elevated white blood cell count,1 but for the purposes of this study, it was defined on histologic basis by the presence of neutrophils in the mucosa, submucosa or muscularis on histopathology. Chronic cholecystitis was histologically defined by the presence of increased lymphocytes in the mucosa, submucosa or muscularis with or without mural thickening or fibrosis.
Statistical analysis
We calculated sensitivity, specificity, PPV and NPV for the various clinical signs and investigations based on histological diagnosis of acute cholecystitis and choledocholithiasis requiring endoscopic retrograde cholangiopancreatography (ERCP). We compared categorical results using a Fisher exact test and continuous variables using a 2-tailed Student t test or the Wilcoxon signed rank test, as appropriate. Statistics were calculated using an Internet-based statistical calculator.18 We considered results to be significant at p < 0.05.
Results:
A total of 107 patients presented during the study period: 69 women and 38 men with a mean age of 55.5 (range 15–91) years. The demographic and clinical characteristics of the study sample are summarized in Table 1. Twenty patients presented twice to the emergency department before their surgery, 2 patients presented 3 times, and 1 patient presented 4 times. The mean number of days from onset of symptoms to surgery was 2.0 (range 0–19) days. The mean number of days from admission to surgery was 1.7 (range 0–11) days. The most common clinical sign was elevated neutrophil count (72%), followed by positive Murphy sign (64%) and elevated total white blood cell count (62%). Almost half the patients had normal liver function tests (LFTs), 16% had elevated results on 4 LFTs, 21% had elevated total bilirubin and 10% had elevated lipase.
Demographic and clinical characteristics of patients included in our study (n = 107)
Table 2 summarizes the imaging findings. All positive findings were included, whether reported by the original or the reviewing radiologist. A total of 83 patients underwent ultrasonography and 28 underwent CT. Seven patients underwent both ultrasonography and CT, and 1 patient underwent both ultrasonography and a hepatobiliary iminodiacetic acid (HIDA) scan. Two patients had known gallstones and did not undergo repeat imaging.
Imaging results
The exact time of imaging studies was not available; only the date was available. Ultrasonography was performed a mean of 1.9 ± 2.9 (range 0–17) days before surgery. Reasons for a delay to surgery included the need for preoperative ERCP and patient comorbidities that precluded immediate surgery. Considering only the 18 patients who were found to have acute cholecystitis on final pathology but in whom ultrasonography did not lead to the condition being diagnosed, 10 had surgery within 24 hours of ultrasonography, and 6 had surgery within 72 hours. A 68-year-old woman had surgery 5 days after a negative ultrasound, and the final pathology was acalculous acute cholecystitis. A 79-year-old woman’s surgery was 5 days after a negative ultrasound because of access issues to the operating room.
Analysis of only ultrasounds yielded 93% interradiologist agreement for cholelithiasis, 88% for dilated ducts or suspected common bile duct (CBD) stones, 92% for pericholecystic edema and 96% for diagnosis of cholecystitis on the ultrasound. Analysis of the 28 CT scans yielded an interradiologist agreement of 71% for cholelithiasis, 89% for dilated ducts or suspected CBD stones, 79% for pericholecystic edema and 79% for cholecystitis. Overall, interradiologist agreement was 92% for ultrasonography and 80% for CT.
Table 3 summarizes the surgical interventions, outcomes and pathology results. Twenty patients required a preoperative ERCP during the same hospital admission. One patient had an ERCP before admission. Four patients needed postoperative ERCP; 1 of them was required after discharge. The mean length of stay was 3.6 days. The mean duration of surgery was 54 minutes. Seven patients needed intraoperative cholangiography, and 4 were converted to open cholecystectomy. There was 1 surgical complication of a retained CBD stone requiring ERCP. There were 11 medical complications: 2 patients had urinary retention, 2 had delirium and 1 each had congestive heart failure, deep vein thrombosis, atrial fibrillation, bronchospasm, chronic obstructive pulmonary disease exacerbation, diarrhea and narcotic-induced hypotension.
Surgical interventions, outcomes and pathology results (n = 107)
There was agreement between the reviewer and the original pathologist in all but 4 cases, where the reviewer found cholecystitis but the original pathologist had not reported it. All patients had histologically confirmed chronic cholecystitis, and 67% had acute cholecystitis as well. A total of 81% had cholelithiasis, and 36% had features of at least focal gallbladder mural necrosis.
Table 4 summarizes the diagnostic accuracy in our study for different clinical variables. No single variable was found to be independently predictive of acute cholecystitis. No single variable achieved an NPV greater than 48%, raising the problem of false-negative tests. The NPV was better for choledocholithiasis, but PPV was relatively poor unless multiple variables were positive.
Diagnostic sensitivity, specificity, PPV and NPV for clinical parameters
Table 5 shows the diagnostic accuracy of imaging studies. Ultrasonography alone was very accurate for diagnosing cholelithiasis (no false negatives) and choledocholithiasis (only 4% false negatives). However, 53% of cases of acute cholecystitis were missed on ultrasounds. Computed tomography alone also had a high incidence of false-negative interpretations. The single patient who had a HIDA scan received a diagnosis of chronic cholecystitis based on the HIDA scan after a negative ultrasound, and the final pathology showed both acute and chronic cholecystitis.
Diagnostic sensitivity, specificity, PPV and NPV for imaging studies
Table 6 shows the diagnostic accuracy of different combinations of imaging and clinical variables. The combination of positive Murphy sign, elevated neutrophil count and cholelithiasis or acute cholecystitis on the ultrasound yielded a sensitivity of 74%, specificity of 62%, PPV of 80% and NPV of 53%.
Diagnostic sensitivity, specificity, PPV and NPV for combinations of diagnostic variables
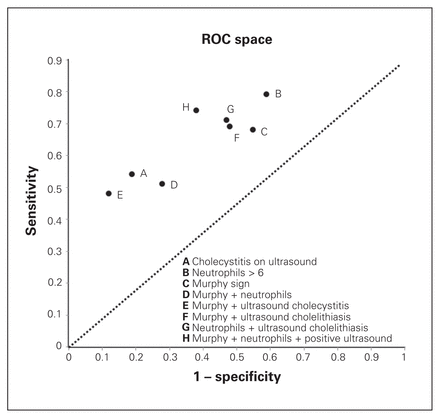
A receiver operating characteristics analysis was performed on selected clinical signs in isolation and in combination (Fig. 1). The signs all fell above the dotted line of randomness. The best clinical prediction was obtained with the “triple test” of positive Murphy sign, elevated neutrophil count and positive ultrasound.
Receiver operating characteristic (ROC) space diagram for select clinical signs.
Wall thickness of 5 mm or more was associated with acute cholecystitis, necrosis and increased duration of surgery (Table 7). Age older than 70 years was associated with increased conversions, complications and length of stay in hospital.
A comparison of ultrasonography outcomes based on measured gallbladder wall thickness and patient age
Discussion
Our findings are in agreement with those of other studies that show ultrasonography is excellent for the diagnosis of cholelithiasis but less so for acute cholecystitis. The NPV of 47% in our study is within the range of 38%–86% reported in the literature.8–12 The addition of CT to ultrasonography did not improve NPV (43%). We found that HIDA was relatively underused yet yielded an accurate diagnosis in the single patient who underwent this technique in our series; HIDA perhaps should be used more often in cases of diagnostic uncertainty, as the literature suggests it has a better sensitivity than ultrasonography for both calculus cholecystitis12 and acalculous cholecystitis.19
With the disappointing ability of ultrasonography to detect cholecystitis, this raises the question of how to manage a patient with right upper quadrant pain and an ultrasound that shows cholelithiasis.
It is interesting that 15 patients with acute cholecystitis had an elevated neutrophil count but normal total white blood cell count. By itself, an elevated neutrophil count had a better PPV and NPV for acute cholecystitis than white blood cell count and positive Murphy sign, but it was not as accurate as ultrasonography.
It is also interesting that every patient had features of chronic cholecystitis. This suggests perhaps a conservative patient selection for emergency surgery, as a more liberal selection would yield patients with normal pathology. It may also reflect a lack of access to elective operating time, as 8 patients presented to the emergency department while waiting for elective surgery. This possibility needs further study. As far as surgical outcomes go, a conversion rate of 4% and surgical and medical complication rate of 1% and 10%, respectively, is in keeping with the rates reported in the literature.20
Some studies show poorer outcomes based on gall-bladder wall thickness20,21 and delayed surgery. Our study showed that wall thickness of 5 mm or more was associated with acute cholecystitis, necrosis and increased duration of surgery, but conversions, complications and length of stay were similar. Of interest, our analysis showed that age 70 years or older was associated with a significant increase in conversions, complications and length of stay in hospital.
Our study agreed with others showing that a delay to surgery of more than 72 hours after admission resulted in a longer total length of stay in hospital (5.4 [95% CI 4.2–6.6] d v. 2.1 [95% CI 1.7–2.4] d, p < 0.05),2–4 but conversions, complications and duration of surgery were similar, contrary to the findings of other studies.5,6 One main case for delay of surgery was the need for preoperative ERCP. Patients needing ERCP had a mean length of stay of 4.9 (95% CI 3.3–6.4) days versus 3.3 (95% CI 2.5–4.0) days in those who did not (p < 0.05).
Conclusion:
We have confirmed that ultrasonography is not as accurate for the diagnosis of acute cholecystitis as for cholelithiasis and that it is vital to also consider clinical paramaters to make an accurate diagnosis. Moreover, we have demonstrated excellent surgical outcomes at our hospital and a potentially useful triad of diagnostic variables to improve diagnosis of acute cholecystitis: an ultrasound showing cholelithiasis or acute cholecystitis, elevated neutrophil count and positive Murphy sign. In equivocal cases or in cases where the patient is difficult to assess clinically, HIDA is underused but potentially helpful.
Acknowledgements
The authors would like to acknowledge Dr. Scott Ainslie, Dr. John Crowley, Dr. Jeff Demetrick, Dr. T. Ghee Hwang and Dr. Kevin Wiseman for allowing their patients to be reviewed in this study. The authors received no funding from any source to perform this research.
Footnotes
Competing interests: None declared.
Contributors: All authors designed the study, acquired and analyzed the data, wrote and reviewed the article and approved the final version for publication.
- Accepted May 28, 2013.